
Neuroanatomy curriculum a vital part of resident education
In July 2021, Neurosurgery Department residents began their new neuroanatomy curriculum. Developed by neurosurgeons Andrew Grande, MD; Carolina Sandoval Garcia, MD; and Andrew Venteicher, MD, PhD, the curriculum is a combination of didactic and hands-on training. It was tailored to the residents’ needs by their colleagues, Sam Cramer, MD, PhD (PGY6); Shiwei Huang, MD, MS (PGY4); and David Freeman, MD, PhD (Chief Resident).

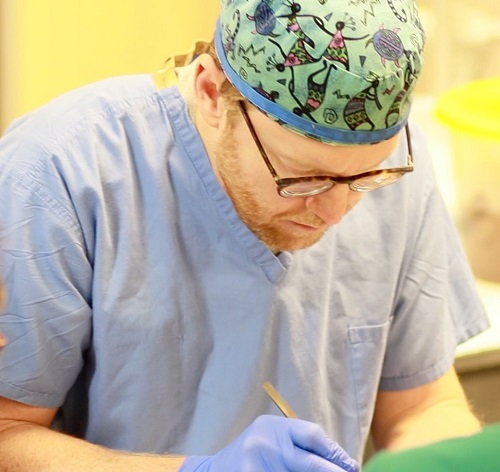
Having access to this type of curriculum and to the Neuroanatomy Lab that supports it is crucial. “A thorough understanding of anatomy is fundamental to being a good surgeon,” said Cramer (pictured here). “Otherwise, you can’t safely correct your patients’ problems. Books are great but they’re two-dimensional. Being able to work in the laboratory with actual specimens is the ideal way to learn anatomy.”
Neuroanatomy is at the core of what neurosurgeons do, according to Grande. “The reality is that the residents are busy and if you don’t establish a formal neuroanatomy curriculum, it’s difficult for them to build in time to get to the lab,” he said. “If they have access on a routine basis, they will use it far more often.”

PGY6 resident Bryan Ladd (pictured here), MD, believes this curriculum is critical. “We have a duty to perfect our skills to the best of our ability, whether it’s through anatomical models such as a cadaver study or through a benchtop wet lab,” he said. “Before we do a surgical procedure in a patient, we want to ensure we’re the best we can be.”
Grande (pictured below working in the lab), who was the leading force behind creating the Neuroanatomy Lab and the resulting curriculum, noted that when he trained at the University of Cincinnati in Ohio, there was an entire culture around neuroanatomy. “People really appreciated it and the lab was a central part of that,” he said. “We would go there a lot and it taught us to be better surgeons.”
The curriculum is structured to focus on a narrow topic, such as cranial neuroanatomy, each month. “We prepare a lecture about the topic, describing its importance from a neurological standpoint,” explained Cramer. “We also prepare several anatomical specimen dissections so we can highlight the structures we’re talking about and demonstrate common surgical approaches to those structures. We’re teaching anatomy in a way that we’ll see it in the operating room.”
The 60 to 90-minute sessions are illuminating. “Even though you think you have a good understanding of a certain piece of anatomy, looking at it from a different perspective can still trick you if you don’t have a complete mastery of the area,” said Cramer. Helping prepare the neuroanatomy labs for the junior residents has been a good experience for him. “It helped me think more about teaching and how much I enjoy it,” Cramer said. “It’s solidified my goal for staying in an academic setting.”
So far, the residents have explored the 12 cranial nerves, as well as the anatomy of and approaches to the lateral and third ventricles of the brain. Upcoming labs will focus on cerebrovascular anatomy.
The residents seem to love the new curriculum. “Speaking for myself, I wish I had had this opportunity during most of my residency,” Cramer said. “It’s a huge improvement in our didactic curriculum.”



