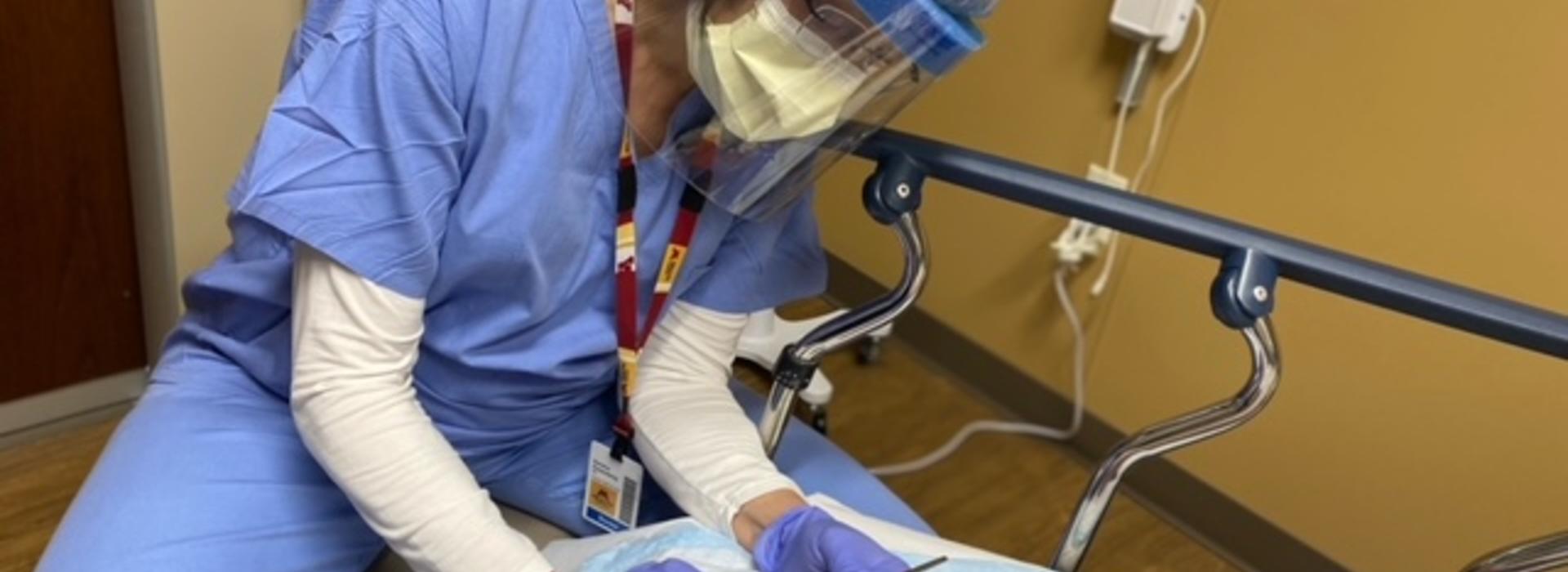
Providing effective, team-based wound care and educating healthcare providers about it meets a huge need
According to Sandra Rosenberg (pictured above), MD, assistant professor and director of Rehabilitation Medicine’s Wound Medicine Fellowship Program, the amount spent annually on chronic wound care in the United States ranges from $30 to $80 billion. To compare, spending on breast cancer care is around $20 billion. “There are more than 6.5 million chronic wound care patients in this country, which is comparable to the number of patients with heart failure,” she said. “It is a big problem.”
One of the elements of that problem is a lack of education about good wound care. Rosenberg began her own education early in her career. When she was 34, she was diagnosed with breast cancer and had surgery. She then developed swelling in the upper part of her arm and no one seemed to know what to do for her. Rosenberg said, “Guess who became the expert?”
Life’s interesting directions
In response to her own condition, Rosenberg learned about lymphedema (swelling in an arm or leg caused by a lymphatic system blockage/damage), which led to increased understanding of the many different contributions to general and peripheral swelling. “Then I got pulled into wound care as most wounds required control of swelling to facilitate healing,” she said. “Life leads us in some very interesting directions.”
Rosenberg would go on to become the first woman elected to the American Board of Wound Medicine Surgery and was certified by that organization in wound care. “Doctors have dropped the ball on wound care,” she said candidly. “A lot of ancillary specialties picked up pieces but often don’t have the high level of clinical expertise to be able to give the best wound care, especially with rapidly changing scientific advancements in wound care today.”
Increasing knowledge
Knowledge about chronic wounds is increasing exponentially, according to Rosenberg. “We are learning about different transmitters in the wound environment, genetics, angiogenesis, and biological markers, along with comorbidities that occur in patients,” she noted. Those comorbidities can include diabetes, obesity, and other medical problems that create issues with healing – not to mention the general aging of the U.S. population.
Good wound care requires a multidisciplinary approach and PM&R (physical medicine and rehabilitation) can play a big role, Rosenberg noted. “To optimize care for chronic wound care patients, providers must coordinate a team of varying specialists in such areas as diabetic care, vascular surgery and medicine, interventional radiology, infectious disease, dermatology, hematology/oncology, nutrition, podiatry, plastic surgery, physical/occupational therapy, and hyperbaric medicine, in addition to rehabilitation medicine,” she said.
Stages of healing
This type of team takes on wounds that don’t heal within three weeks, which makes them chronic. According to Rosenberg, there are four main stages of healing:
- Hemostasis (stopping the bleeding, first 1-6 days)
- Inflammation (within six days, white blood cells come in to clean out the “garbage”)
- Proliferation (within two weeks, the body sends out fibroblasts to lay down a matrix to close the wound)
- Remodeling (the initial collagen that was laid down is very unstable and stronger types of collagen are sent in to replace it. This can take up to about one year.)
Getting the wound closed and as strong as possible often takes up to two years. “Chronic wounds tend to get stuck in the inflammatory stage. This can be from issues such as trauma, lack of oxygen, immunosuppression, poor nutrition, infection, foreign bodies, or systemic disease,” said Rosenberg. “To treat these wounds, the provider must become a detective to discover what is going on.”
Dealing with bacteria

First, the team makes sure there isn’t a significant arterial component, underlying vasculitis disease (inflammation of the blood vessels), cancer or unusual skin disease. A detailed exam is done with review of history, medications, labs, imaging, previous treatments, and allergies to help determine why the wound is there and what may contribute to its being chronic. “Most of the wounds we see are venous wounds,” said Rosenberg (pictured at left). “When arterial status is found to be adequate for healing, the wound is usually numbed and debrided. This cleans out dead tissue that contributes to continuing inflammation.”
Debridement also helps return the wound to a more acute state. “In more than 80 percent of chronic wounds, a protective shield called a biofilm is formed around the bacterial community,” explained Rosenberg. “Most forms of antibiotics can’t often defeat that.” Debriding disrupts the biofilm. Antimicrobials, many times used in dressings, help prevent biofilms from reforming.
Then you need to decrease any swelling. “Extra fluid tends to get into the middle layer of the skin, pushing the top layer away from the lower arteries that supply oxygen and nutrients,” said Rosenberg. “Decreasing that swelling helps improve oxygen and nutrient supply to the upper layers of the skin and promotes healing.”
Rosenberg often quotes Albert Einstein — Doing the same thing over and over again and expecting different results is the definition of insanity — to describe the current state of wound care in many medical settings. To her, it’s simple. “If a wound isn’t healing, get the patient to someone who really knows wound care,” she said. “We have wounds that come in and someone has been treating them with gauze and bacitracin for three years. If a wound doesn’t have a significant arterial component, keeping them warm and moist works much better — not wet because you wash away all the new healing factors and can damage the surrounding skin — and not dry as that inhibits the capillaries from bringing in nutrition and oxygen. Also, when you remove the dry covering, it’s painful and takes out all the fresh, new, fragile components that are trying to rebuild the skin.”
A better future
Rosenberg wants the future to be better for wound care patients. “Family practice residents at the U come through and learn about wound care,” she said. “But a lot of the medical community doesn’t get this type of training.” One of her goals – and that of the Rehabilitation Medicine Department – is to establish a one-year fellowship in wound care at the U that will be offered to start one candidate in academic year 2022-2023, beginning hopefully in January. “I want our fellow to have the opportunity to get the training I would have loved to have,” she said.
To increase its own wound care capacity, the Rehabilitation Medicine Department recently added Cancer Care Director Florence John, MD, MPH, to the team as well as a certified nurse practitioner with extensive experience in wound care. Rosenberg is also helping at the national level to get the wound care subspecialty recognized by the American Board of Medical Specialties and/or the American Board of Osteopathic Medicine to help ensure that the new fellowship can eventually be accredited.
“The bottom line is that all these patients are suffering,” said Rosenberg. “They may lose limbs and many even lose their lives. The quality of their lives has certainly been impacted. Despite all this, wound care education has been neglected. I believe we’re taking a step in the right direction to help rectify that.”



