Using the most cutting-edge technology to advance the care of brain tumor patients
When Madelyn Lauer’s headaches crossed the line from being the result of fatigue to something more, she scheduled an appointment with a neurologist and requested an MRI of her brain. She just wanted to understand what was happening; she certainly didn’t expect a brain tumor to show up on the imaging.
As she and her husband, Zach, who is a faculty member of the U’s Internal Medicine Department, discussed what to do, they conferred with his medical colleagues and the name of Neurosurgery Department Head Clark C. Chen, MD, PhD, came up. “They had heard about him and his work with brain tumors and recommended him highly,” said Madelyn. “We feel very fortunate to have found someone who has as much expertise as he does.”
Gave us options

During their first consultation, Dr. Chen walked Madelyn and Zach (pictured here, photo by DnK Photography) through her imaging thoroughly. “He talked about what the brain tumor might be, what we could do, and gave us options for moving forward,” said Madelyn. “He also recommended that we have all the information before choosing the treatment.”
Madelyn and Zach appreciated Dr. Chen’s emphasis on maintaining quality of life while aggressively treating her tumor. “He helped us understand some of the strategies that could address my problem,” said Madelyn. “We felt that we had a well-rounded recommendation from him and his team and set a goal of working together.”
Madelyn’s tumor resided in the region of her brain that controls her memory, speech, and right-hand and leg function. “Any injury to the normal brain in this region will significantly diminish Madelyn’s quality of life,” commented Chen. “But there was no doubt that the tumor needed to be removed.”
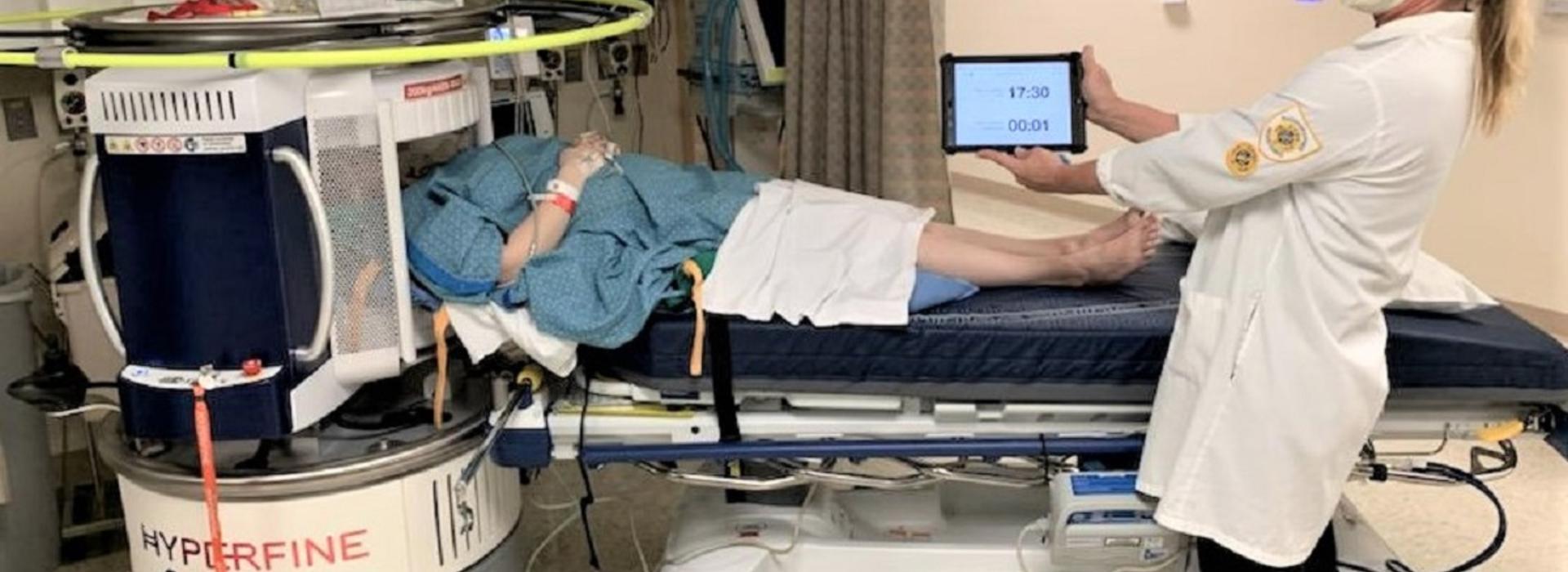
There were three priorities for Dr. Chen as he considered her surgery – preplanning the procedure for an optimal outcome, keeping Madelyn awake during the surgery to minimize risk of injury to normal brain tissue adjacent to the tumor, and using a new portable MRI machine following the resection to assess the surgical outcome. Madelyn would make history as the first M Health Fairview patient to have post-operative images recorded by this new machine.
Priority #1: preplanning
“Surgeries begin well before the surgeon walks into the operating room,” said Dr. Chen. “I create computational, three-dimensional models of the tumor and the adjacent normal brain. These models enable me to practice my surgical maneuvers before the actual procedure.” Dr. Chen noted that this process ensures there are no surprises during the surgery. He uses the movie, “Sully,” as an example. “Landing his disabled jetliner in the Hudson River was a daunting task,” said Dr. Chen. “But Captain Sullivan had participated in many disaster simulations that enabled him to be prepared for this situation. Like Sully, the pre-planning we do as surgeons is critical to a successful surgery.”
Priority #2: keeping Madelyn awake during surgery
Because of the location of Madelyn’s tumor, it was necessary that she be awake during the surgery. “For her type of tumor, it’s often difficult to tell where it ends and normal brain tissue begins,” said Dr. Chen. “I do the surgery while the patient is awake to ensure we do not damage the surrounding brain. I do this frequently, but it does require a specialized skillset and a dedicated support team.”
During the procedure, the surgical team interacted with Madelyn. “I was participating throughout the process, which sounded scary beforehand, but was so important,” she said. “They asked me questions and had me do certain things to make sure they were protecting everything we discussed before the surgery. The team was so supportive – if I had an itch I couldn’t scratch, they would take care of it.”
Priority #3: assessing surgical outcome with a portable MRI machine
M-Health Fairview is one of a handful of institutions in the United States that has access to the Hyperfine Swoop® mobile MRI technology. It was used for the very first time with Madelyn. The machine was wheeled into the Post Anesthesia Care Unit (PACU) for immediate imaging of her brain after her surgery. “Having the machine right there also meant I could stay with my supportive PACU nurse,” said Madelyn.
“With any surgery there are risks,” added Zach. “Being able to get MRI information so quickly after the procedure helped rule out the complications that may come with a surgery like this.”
The Hyperfine machine uses a lower-strength magnetic field coupled with artificial intelligence (AI) to construct images of the brain, according to Dr. Chen. “Because of this lower field strength, a patient can safely undergo an MRI in the presence of family and friends for the entire duration of the study. Moreover, the information garnered from the MRI can help guide my post-operative care recommendations.”
Road to recovery
Madelyn is now on the road to recovery. Her headaches are better, and she has started her follow-up chemotherapy and radiation. “We definitely had a good outcome with Dr. Chen and his team,” she said. “We’re looking forward to the future and are hopeful moving through the next steps.”
Zach noted that Madelyn’s diagnosis inspired them to re-evaluate how they spend their time and where they put their effort. “As a provider, it gives you a different understanding of the patient experience and makes you think more about having a well-rounded team that considers the patient’s preferences as well as bringing the best knowledge and expertise to the situation,” he said. “Throughout this entire experience, everyone listened to us when we brought up a concern, question or thought.”
Dr. Chen added that, “Because of the technologies available at M Health Fairview, I am confident that we were able to achieve the best possible surgical outcome for Madelyn. I believe that her future looks bright and anticipate that she will be able to return to pursuing her passions and living a very fulfilling life.”



