Artificial Pancreas Oxygenation Monitored
Scientists at the University of Minnesota have spent years developing a bioartificial pancreas, adapted from a commercially available product. The implantable device is meant to contain insulin-producing islet cells to replace the nonfunctioning or nonexistent native islet cells for someone with type 1 diabetes.
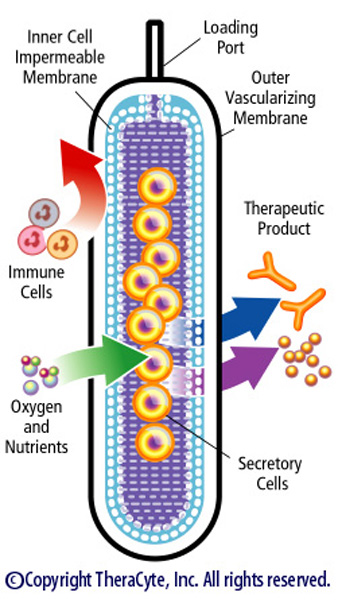
The bioartificial pancreas in development at the U of M is adapted from the TheraCyte system, a device fabricated from membranes which protect implanted cells from rejection and induce the development of capillaries. (Photo courtesy of TheraCyte, Inc.) With critical support provided early on by private philanthropy, a team of investigators at the University’s world-renowned Center for Magnetic Resonance Research (CMRR) is now working on an innovative new method that will help doctors know whether the cells within the device are getting the oxygen they need. The team, led by radiology professor Michael Garwood, Ph.D., includes graduate students Brad Weegman and Sam Einstein.
“What we’re doing is measuring the oxygen noninvasively, using one of the most powerful MRI (magnetic resonance imaging) systems we have,” explains Weegman. With the help of magnetic resonance spectroscopy, the technique measures the total average oxygen inside the device.
