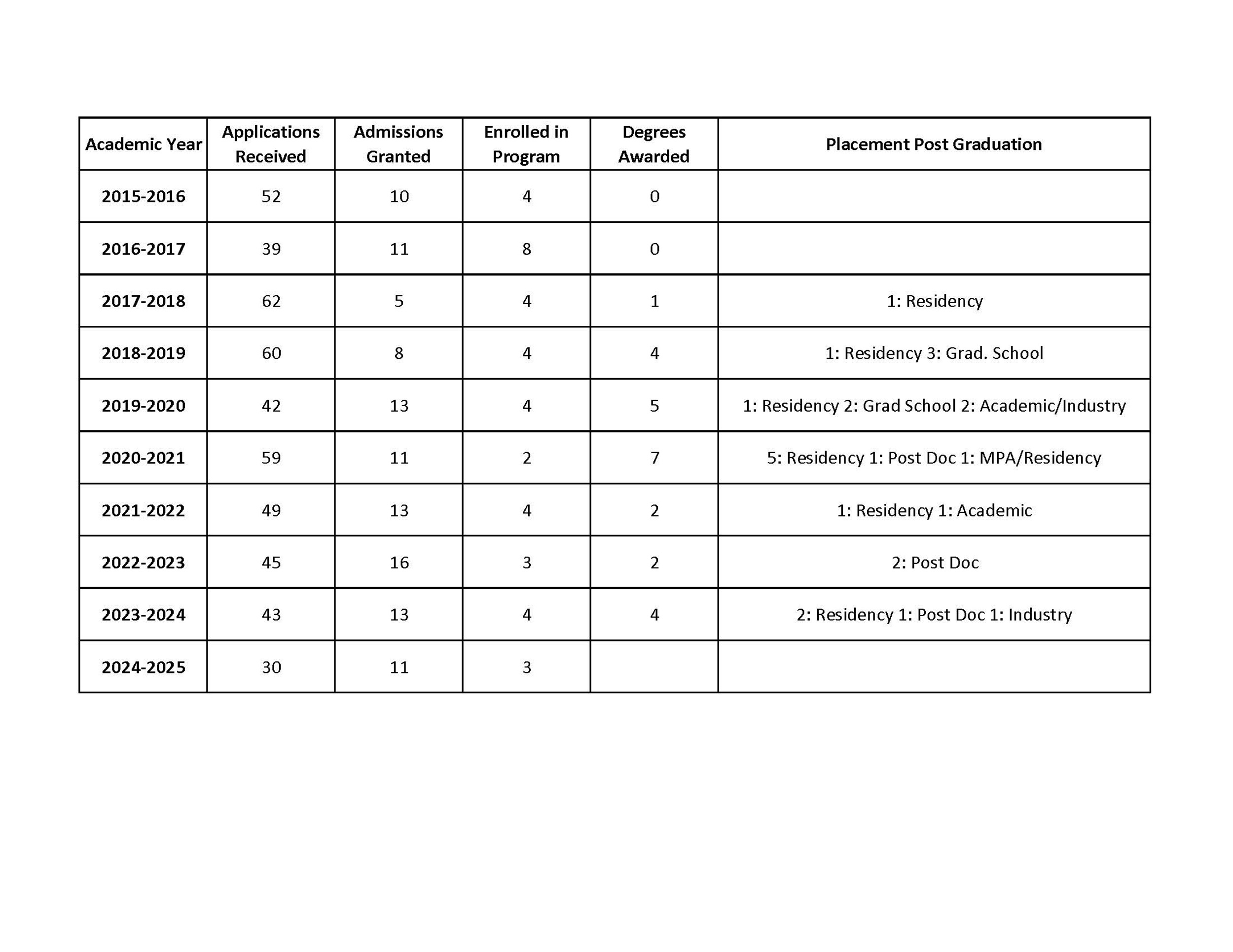
Medical Physics Graduate Program
The Medical Physics Graduate Program is accredited by the Commission on Accreditation of Medical Physics Education Programs (CAMPEP) and offers MS and PhD degrees.
The goal of the program is to prepare students for entering a clinical medical physics residency program in therapy or imaging physics and/or to pursue a career in research and teaching in radiation therapy, radiology, or magnetic resonance imaging.
The program meets the requirements of the Graduate School of the University of Minnesota, AAPM Reports 197, 197S, and the CAMPEP Standards for Accreditation of Graduate Educational Programs.
The Medical Physics Graduate Program generally admits students in the Fall semester. This program does not grant conditional admissions. Deadline for Fall 2025 admissions will be January 5, 2025.
What is Medical Physics?
Medical physicists are professionals with education and specialist training in the concepts and techniques of applying physics in medicine. Medical Physicists work in clinical, academic or research institutions. (Source: IOMP)
Medical physicists are concerned with three areas of activity:
- Clinical service and consultation in radiation oncology and radiology departments
- Research and development in areas such as cancer, heart disease, and others
- Teaching medical physics students, resident physicians, and radiology and radiation therapy technology students
(Source: AAPM)
AAPM's public education web page describing medical physics:
https://www.medicalradiationinfo.org/medical-physics/
AAPM's public education web page describing a career in medical physics:
https://www.medicalradiationinfo.org/careers/
Program Governance
The program governance includes the Director of Graduate Studies (DGS), the Steering Committee, and the Admissions Committee. The Steering Committee addresses the long term needs of the program and any short term issues. The Admissions Committee reviews applications for admissions and makes admissions decisions.
The majority of the instructors for the program are from the Departments of Radiation Oncology and Radiology at the University of Minnesota. Faculty are listed as full if they advise and support student(s) in the program at least once every five years, actively participate in the program by serving on student(s) MS and PhD committees, teaching courses, or serve in one of the graduate program committees.
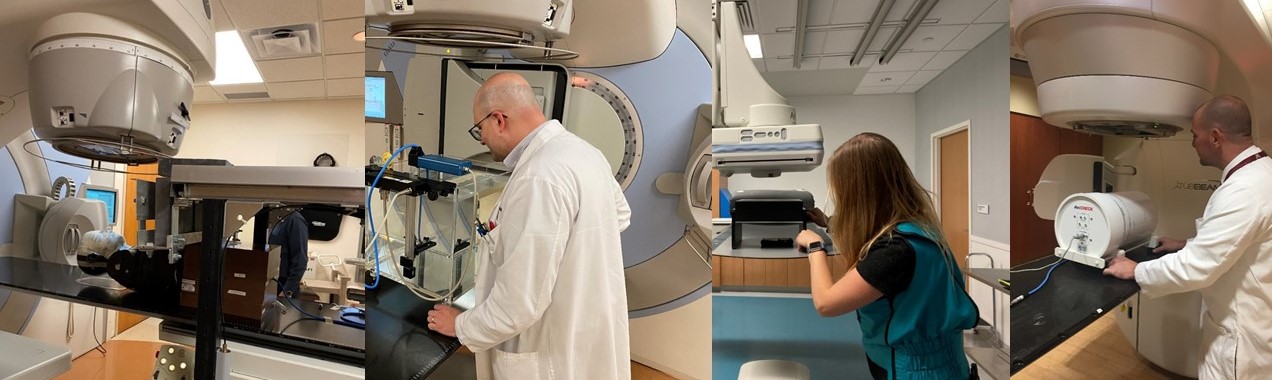
Facilities
The facilities and clinical equipment of the University of Minnesota Medical Center are available to the faculty and students of the graduate program in Medical Physics. These include departments of Radiation Oncology and Radiology, including The Center for Magnetic Resonance Research.

Additional facilties within various University of Minnesota departments and centers are also available to graduate students as needed.
The full resources of the University of Minnesota Library systems both online and its physical holdings are available to all graduate students of the University of Minnesota. Other materials not directly accessible within the University of Minnesota Library system can be acquired via interlibrary loan.
Read a general description of the University of Minnesota Libraries.
Read about particular library services offered to graduate students.
Active Research Projects
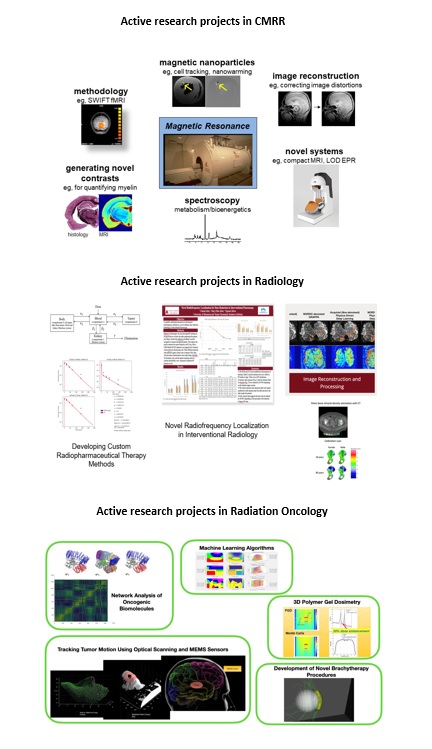
Recent Student Publications and Presentations
Recent Publications:
N. Becerra-Espinosa, L. Claps, P. Alaei, Comparison of visual and semi-automated kilovoltage cone beam CT image QA analysis, J. Appl. Clin. Med. Phys. e14190 (2024)
S. Fakhraei, E. Ehler, D. Sterling, L.C. Cho, P. Alaei, A Patient-Specific correspondence model to track tumor location in thorax during radiation therapy, Phys Medica 116 (2023)
N. Zulkarnain, A. Sadeghi-Tarakameh, J. Thotland, N. Harel, Y. Eryaman, Aworkflow for predicting radiofrequency-induced heating around bilateral deep brain stimulation electrodes in MRI, Med. Phys. (2023)
A. Sadeghi-Tarakameh, L. DelaBarre, N. Zulkarnain, N. Harel, Y. Eryaman, Implant-friendly MRI of deep brain stimulation electrodes at 7 T, Mag. Reson. Med. (2023)
E. Torres, P. Wang, S. Kantesaria, P. Jenkins, L. DelaBarre, D. Cosmo Pizetta, T. Froelich, L. Steyn, A. Tannús, K. Papas, D. Sakellariou, M. Garwood, Development of a compact NMR system to measure pO2 in a tissue-engineered graft, J. Magn. Reson (2023)
T. Froelich, L. DelaBarre, P. Wang, J. Radder, E. Torres, M. Garwood, Fast spin-echo approach for accelerated B1 gradient–based MRI, Magnetic Resonance in Medicine (2023)
AAPM 2024 Presentations:
A. Monsef, P. Sheikhzadeh, J. Steiner, M. Elhaie, M. Fooldai, F. Sadeghi, Optimization of Ga-68 Dotatate Activity for Oncologic PET Imaging: Phantom and Patient Study
A. Alshreef, M. Assalmi, T. Allen, B. Rogers, C. Oare, C. Ferreira, “Dose to brain versus dose to water for GammaTile implanted brachytherapy”
A. Alshreef, M. Assalmi. T. Allen, B. Rogers, C. Oare, F. Jafari, C. Ferreira, “Dose Heterogeneity Simulation for Permanently Implanted Cs‑131 Seeds for Brain Tumor Brachytherapy”
T. Adhikari, A. Alshreef, C. Ferreira, "Dose Coverage and Dose to Organs at Risk for GBM Patients Treated with Gammatile"
S. Pani, B. Nguyen, D. Mathew, Y. Watanabe, “Preliminary Evaluation of Hall Effect Sensor Array for Patient Motion Tracking”
S. Lee, Y. Watanabe, "Prediction of Heterogeneous Treatment Planning in Gamma Knife Radiosurgery Using Homogeneous Plan with Conditional Generative Adversarial Network
ISMRM 2024 Presentations:
S. Lee, F. Branzoli, O. Andronesi, C. Chen, A. Lin, R. Liserre, G. Melku, T. Nguyen, M, Marjanska, Analysis of MRS voxel placements in brain tumors performed by MRS experts
N. Zulkarnain, A. Sadeghi-Tarakameh, D. Koski, N. Harel, Y. Eryaman, In-vivo Validation of a Workflow to Predict Heating around a Deep Brain Stimulation Contacts
ABS 2024 Presentation:
C. Ferreira, D. Sterling, S. Zhang, M. Reynolds, K. Dusenbery, L. Sloan, A. Alshreef, C. Chen, Gammatile Cs-131 Permanent Brain Implants: From Clinical Implementation To Treatment Outcomes And Beyond
Program History
This graduate program was started as an interdisciplinary graduate program under the name Biophysical Sciences in the 1950s by Dr. Otto Schmidt to encourage collaboration among biologists, chemists, and physicists. Then, as now, faculty had their salaried appointments in various home departments, including departments within the Medical School, but participated in Biophysical Sciences because of their interests in collaborative, interdisciplinary projects.
By the late 1960s and early 1970s, disciplines such as biophysics, biochemistry, physical chemistry, etc. were established in the mainstream, so the emphasis in Biophysical Sciences shifted to health informatics (integration of computers for modeling and data base analysis) and medical applications of biochemistry with Dr. Gene Ackerman and Dr. Russell K. Hobbie as Directors of Graduate Studies.
By the late 1980s the computerization of all disciplines had become routine and most of the faculty had minimized their participation in the Biophysical Sciences Program. At about that time, however, a resurgence of interest in applications of various disciplines to problems in “radiologic sciences” – medical imaging, radiation therapy, and radiobiology – resulted in a renewal of interest in the program. In the US, the field of radiologic science is known as a profession by the term “Medical Physics”. Thus, by the early 1990’s the emphasis of the program had shifted to Medical Physics. In 1993, the program underwent an internal review under the direction of Associate Dean Kenneth Zimmerman at the request of Vice President and Dean Anne Petersen. The purpose of the review was to explore the future of involvement of the Medical School in the program. E. Russell Ritenour, became Director of Graduate Studies at that time.
In 2012, the name of the Biophysical Sciences and Medical Physics program was changed to Medical Physics to more closely align the name of the program with the focus of the majority of the students in the program. The program as it currently stands focuses on Medical Physics but does not preclude the student from having a graduate project that is outside the traditional borders of Medical Physics. This is due to the fact that there are several professors associated with the program that have interests aligned with Medical Physics that are not purely clinical in focus. To aid in this transition of the program and to promote the accreditation process, Bruce J. Gerbi, PhD was installed as the Program Director. Upon retirement of Dr. Gerbi, Parham Alaei, PhD was elected as program director in May 2017.
For specific program information, please contact:
Parham Alaei, PhD, Professor
University of Minnesota Medical School
Department of Radiation Oncology
612-626-6505
alaei001@umn.edu
Mayo Mail Code 494
420 Delaware Street SE
Minneapolis, Minnesota 55455