Fourth-year Resident Wins at AAOS, Works to Increase Medical Student Interest in Orthopedics
FOR LAUREN CASNOVSKY, MD, PGY-4, orthopedics has always been a passion. As a child she had metatarsus adductus, a common foot condition that causes the front half of the foot to turn inward, which wasn’t corrected with casting. This resulted in her first orthopedic surgery. “I knew since I was five that I wanted to be an orthopedic surgeon,” she recalls.
Casnovsky took an active role in her pursuit of an orthopedic career, and in high school volunteered at Gillette Children’s Specialty Healthcare to get hands-on experience. Although she approached medical school open to other specialities, nothing could replace her desire to be an orthopedist. Casnovsky’s story isn’t the norm. “Women in Orthopaedic Surgery,” published in the Journal of Bone and Joint Surgery, found that female medical students don’t typically enter medical school with the intention of becoming an orthopedist, while their male counterparts do. It’s possible that the delayed exposure to orthopedics in medical school may deter women from the specialty. “There’s this huge push to have more outreach for women in medical school because they don’t know if they want to do ortho yet,” Casnovsky says. “I’m sort of an outlier in that way, because I’ve always known, and everything I’ve done has been deliberate to get here.”
In her first years of medical school, Casnovsky connected with Ann Van Heest, MD, professor and residency program director, to collaborate on a chart review of acquired upper extremity growth arrest. “I remember spending my Sundays at Gillette doing chart and x-ray review with Erich Gauger, the chief resident at the time, and I think that’s part of what landed me here,” she recalls. All of her hard work volunteering and seeking additional opportunities in orthopedics paid off, and in 2016 she started residency at the University of Minnesota Department of Orthopedic Surgery, where she has become a leader among her peers.
"Since I met her as a medical student, Dr. Casnovsky has demonstrated a passion for orthopedic surgery,” says Van Heest. “She is a hard-working resident who takes excellent care of her patients in addition to being genuinely interested in helping others. Lauren has excelled as a resident clinician, researcher, and teacher." Her research garnered national recognition at the 2019 American Academy of Orthopaedic Surgeons (AAOS) annual meeting where she won best trauma poster. Five posters per subspecialty area are chosen for presentation in advance, including submissions from practicing orthopedic surgeons, and only one is selected as the winner.
Although she plans to pursue a subspecialty in hand and upper extremity after graduation, her interest in trauma inspired her to partner with a research team at Regions Hospital to develop her poster theme, “Trend and Economic Implications of Implant Selection in the Treatment of Intertrochanteric Hip Fractures: A Review of the American Board of Orthopaedic Surgery Database 1999-2017.”
“Lauren was incredible to work with on this project,” says Brian Cunningham, MD, assistant professor and project co-author. “She took initiative, worked diligently with the ABOS (American Board of Orthopaedic Surgery) to collect data, and spent hours reviewing the poster and manuscript. She demonstrated the tenacity that it takes to move research from an idea to a nationally awarded presentation. Our research team at The Value Initiative is so proud of her and look forward to following her career.”
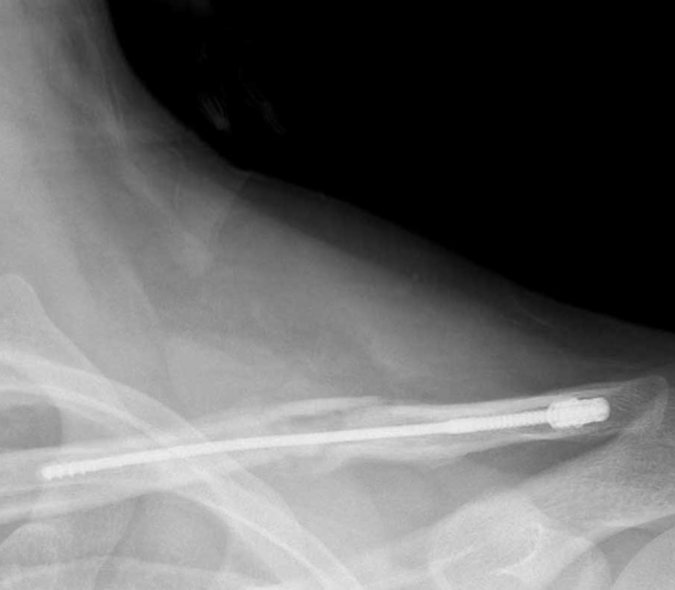
Their research analyzed the economic impact of using sliding hip screws (SHS) versus intramedullary nails (IMN) in the treatment of intertrochanteric hip fractures. The gold standard to fix this type of stable hip fracture is a sliding hip screw, which has been around since the seventies. After the turn of the century, intramedullary nails became increasingly popular and are now used in the vast majority of cases. “The problem is that nails are much more expensive,” Casnovsky explained. “Depending on the hospital system, it can be two to three times the cost of a sliding hip screw.”
The caveat is that not all intertrochanteric hip fractures can be treated with a sliding hip screw, and some residency programs aren’t even teaching students how to use one. “I think we’re kind of spoiled here because we’ve got Dr. Swiontkowski driving the evidence-based medicine and using meta-analysis and randomized control trials to show that there is no difference between the two implants for a simple stable, intertrochanteric hip fracture,” Casnovsky added.
While her data shows a steep rise in IMN usage over the last decade, she acknowledges that they don’t have access to the x-rays from patients with the fractures. Because of this, there is no way to determine whether a simple or complex fracture occurred and if an SHS could have been used in lieu of an IMN. While in the grand scheme of things implants don’t make up the bulk of the cost of these surgeries, Casnovsky extrapolated that the healthcare system could have saved roughly $793 million from 1999-2017 had an SHS been used when deemed appropriate. “The difference is that if you don’t learn how to use a sliding hip screw during residency, you’re likely not going to use one in practice,” she explained. “If you’re trained in both, you can be skilled in both.”
Apart from her achievements at AAOS and advocacy for value-based healthcare, Casnovsky also received the Resident as Teacher Award presented annually during resident graduation. The award recognizes residents that actively teach and mentor medical students. “It was really nice because I remember what it was like to be a medical student; it’s not glamorous and you feel like you’re in the way and you don’t know anything,” she says. “I don’t feel like I went out of my way to include the students, but I do try to make people feel welcome and teach them.”
Some of the medical students that Casnovsky mentored have ended up pursuing a residency at the U of M. Melissa Albersheim, MD, PGY-1, was a co-author on the winning AAOS poster and was also one of Casnovsky’s medical students at Hennepin Healthcare. As a third-year medical student leaning towards orthopedic surgery, she says that Casnovsky always took time out of her busy schedule to answer questions and help her through the process. “She has had an immense impact on me in terms of pursuing orthopedics,” Albersheim says. “She is the ultimate role model and will take the time to actively teach junior residents and medical students even if she’s exhausted. I strive to be like her in multiple ways, to be able to make time for important relationships outside of work and be a successful mentor and teacher for students and junior residents.”
Casnovsky says that she’s just carrying on the legacy of mentors and resident educators that came through the program before her. “I think I’ve had a lot of really good mentors who have helped me, the type of people who show interest in your education. That’s who I want to be like.”