Knowing When it’s Time to Get Something Done About Your Back Pain
How do you know when your back pain is just too much? When you can no longer pick up your grandchildren. St. Paul, Minn., resident Susan Grande (pictured at right), an active, trim 67-year-old, was stopped dead in her tracks by back pain. For several months, she tried different ways to mitigate the pain, from physical therapy to bracing to medication. But the problem persisted.
It all started in October of 2016 when Susan’s knees started bothering her and then her back began acting up. “The chronic pain was fatiguing and my energy was down,” she said. “I was spending a lot of time on the couch. I felt I was on a downward course and gathering speed.”
After the unsuccessful therapies, her son, U of M neurosurgeon Andrew Grande (pictured at right), MD, advocated surgery. He recommended that it be done by a university colleague, orthopaedic surgeon and Neurosurgery Professor David Polly, MD. Grande accompanied his mother to her first appointment with Polly.
“It is an honor to be chosen by a colleague to treat a beloved family member – it’s the ultimate vote of confidence,” Polly noted. In Susan’s case, she had two physician advocates – Andrew and her husband, Tom, who is an obstetrician/gynecologist. Her daughter is also a physician. “Susan’s appointments tended to go a little longer than usual because her family members asked appropriate, intelligent questions,” said Polly.
Minimally invasive treatment
During the appointment, Polly explained that Susan had isolated L [lumbar] 2 and 3 disc degeneration collapse and retrolisthesis, an acute spine condition in which a single vertebra gets displaced and moves backwards onto the vertebra lying immediately below it. Polly felt there was a good combination of minimally invasive techniques that would work for Susan.
“Dr. Polly did an excellent job describing the problem clearly, and honestly characterizing the possibility of surgical success or failure,” said Susan. “Afterwards, Andrew talked at length with both my husband and me. He recommended that I should have the surgery.”
On January 9, 2017, she had the procedure. The first small incision (1.5”) would be through her side. “With fluoroscopic and EMG [electromyography] control, we did what’s called a transpsoas approach,” Polly (pictured at left) said. “We cleaned out the disc, elevated it back up to where it was supposed to be, and put in a plastic spacer with bone morphogenetic protein in it.” The spacer would encourage “fusion,” or bone growth, to strengthen both it and the surrounding vertebra.
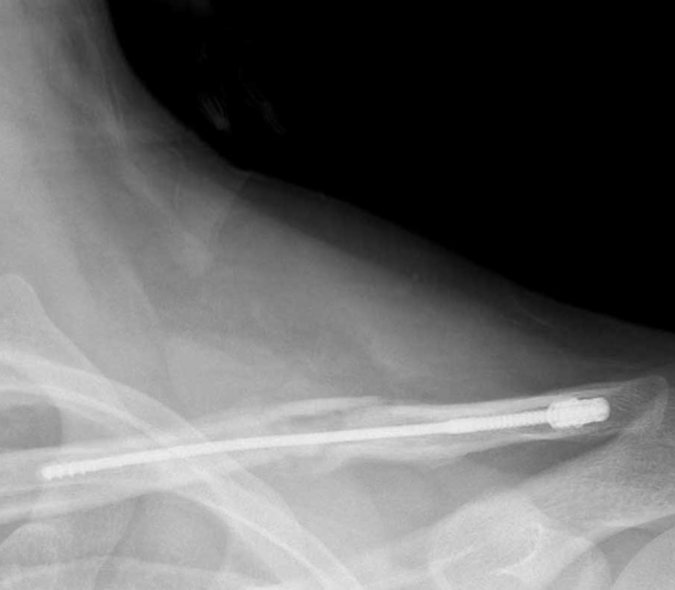
Then the surgical team turned Susan over and used image-guided technology to go through her back and place percutaneous pedicle screws at the L2-3 level for additional stability. “The blood loss during this surgery was minimal,” noted Polly. “We didn’t really denervate any muscles, either, which worked well for her.”
Susan had a couple of advantages going into the surgery. “She was in great shape before this happened,” Polly pointed out. “Her issue was at a higher lumbar level – you can’t do this procedure below L4.” He added that the surgical team used state-of-the-art techniques to solve Susan’s problem while sparing her muscles.
World-renowned
In fact, the U’s Orthopaedic Surgery Department is a world leader in using these techniques, particularly the use of the OR CT scanner and the stealth navigation technology. “We’ve published at least 10 articles about this topic,” Polly noted. “I’ve spoken about it around the world. I was recently invited to Beijing to talk about it at the oldest Western hospital in China.”
Susan had the surgery on a Monday and came home Saturday. Afterward, a team that included a nurse practitioner, occupational therapist, and physical therapist was sent to her home. “They came twice a week for three weeks,” Susan said. “That was invaluable. All three were just superb and played a key role in my recovery.”
Some of the training provided by the team included the importance of proper posture and body movement, how to roll, and how to get in and out of bed. “The physical therapist worked with me over the six visits to reprogram myself about how to move to avoid bending and twisting,” Susan noted. “I can’t say enough good things about the team.”
She was also given several different kinds of exercises to do. “I was motivated to get as well as I could,” said Susan. “By the end of three weeks, I was well on my way to doing the core strengthening exercises.”
Fully recovered
During her follow-up visit in May, Polly assessed Susan’s pain using the Oswestry Disability Index. “The best possible score is 0, the worst is 100,” he said. “Before the surgery, she was a 48; during the follow-up, she was below 20.” Polly believes that Susan was essentially fully recovered at that point. “The X-ray showed that the bone had healed; it looked excellent,” he said. “We felt she could go back to doing anything she wanted to do.”
Susan might never have chosen the path to surgery. “If I hadn’t had Andrew in my life, I may have just accepted that I had degenerative disc disease and thought it was a natural part of ageing,” she said. “I encourage anyone in my position to explore all their options and if they decide on surgery, to seek out an expert in this type of procedure.”
Susan is pretty much back to doing the things she loves to do and most importantly, picking up her grandchildren again.