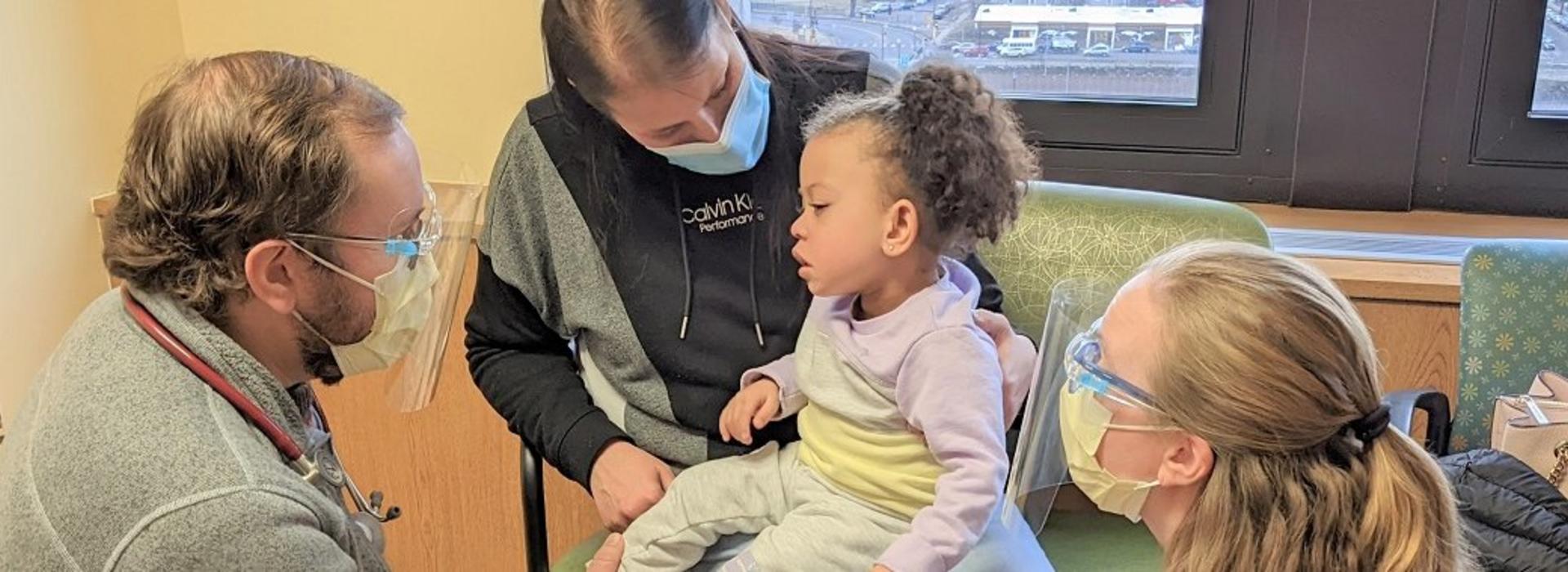
Getting involved early, working with the right providers is key to ensuring that kids with cerebral palsy can thrive
According to the Centers for Disease Control, cerebral palsy (CP) is a group of disorders that affect a person’s ability to move and maintain balance and posture. CP is the most common motor disability in childhood. Cerebral means having to do with the brain. Palsy means weakness or problems with using the muscles. CP is caused by abnormal brain development or damage to the developing brain that affects a person’s ability to control their muscles.
“It’s something that happens as the result of an injury to the developing brain before, during, or shortly after birth,” said Assistant Professor John Fox, DO, director of the Pediatric Rehabilitation Medicine Program. “The injury causes changes to muscle movement that often affects a child’s development.”
Many causes
Fox noted that the damage can be from a brain hemorrhage, lack of oxygen, decreased blood flow to the brain caused by a clot, infection, inflammation, or abnormal brain development. There might also be an underlying genetic condition that changed the developing brain. “The damage occurs from a static lesion, so the injury doesn’t progress or worsen,” Fox said. “It’s lifelong and there is no cure or preventive measures for it, but there are treatments and therapies we can provide to improve the health, functioning, and well-being of children diagnosed with cerebral palsy.”
All people with CP have problems with movement and posture, he noted. Many also have related conditions such as intellectual disability; seizures; problems with vision, hearing, or speech; changes in the spine (such as scoliosis); or joint problems (such as hip dysplasia or joint contractures).
The number one risk factor for cerebral palsy is premature birth (being born before 37 weeks).

Not everyone with CP is diagnosed right away. “As a PM&R doctor, I like to be involved as soon as possible in a child’s development,” said Fox (pictured here). “That can even be before cerebral palsy is diagnosed. Sometimes the symptoms are present early in life; sometimes, it’s not as apparent until the child is growing, and we start to notice delayed motor milestones.”
Fox takes a holistic approach to working with his CP patients, looking at gross and fine motor skills and how the child is developing overall. He checks to see if they have high muscle tone (spasticity), which is often the case with cerebral palsy. He also wants to know if the child is able to roll, crawl, pull to stand, or walk. As part of his care, Fox does a comprehensive history of the child, making sure they’re connected to the appropriate resources.
Stretching, stretching, stretching
“Some patients may need rehabilitation, such as physical, occupational, or speech/swallow therapy,” he said. “Stretching is the primary method of treating increased muscle tone in these patients. I work with families and therapists to make sure we have a good stretching and positioning program in place.” Fox emphasizes how important stretching is because when the patient loses any range of motion, it’s sometimes hard to get it back. “Stretching helps with positioning, it helps with comfort, it helps with function,” he said. “What’s one of the most important things in CP therapy? Stretching, stretching, stretching.”
Fox can also treat these patients using medications or injections of botulinum toxins (such as Botox) to help relax the muscles, or with phenol injections, which help limit signals sent from the nerves to the muscles that cause contractions.
Cerebral palsy can affect other aspects of life such as sensation, communication, behavior, and it can lead to hip subluxation or pain due to muscle tightness, drooling, and bowel and bladder changes. “We make sure we address all those things, using a teamwork approach,” said Fox. “I work closely with the Rehabilitation Therapists, Neurology, Orthopedics, and the Complex Care Team, as well as the primary care doctor and the child’s family.”
Child will show you
Brain imaging is often used to help diagnose cerebral palsy. “There are certain characteristics you can see on an MRI that are associated with cerebral palsy,” said Fox. “There are also some physical measures we can use to predict function down the road and how independent a child might be, but it can be tricky. As they grow, the child will show you where they need help and where they don’t. We tailor the treatment plan to each patient to help them become as functionally independent as possible.”
Sometimes CP patients need orthotics, so Fox makes sure they’re connected to an orthotist to get what they need to help improve function and maintain joint positioning. They may also need other adaptive equipment such as standers, wheelchairs, or gait trainers. “There is a wide range of things we can do to help these kids and their families,” said Fox. “A rehab doctor is a great point person to ensure that kids with CP are connected to everything they need. We want to help them thrive.”
People with CP can have fulfilling lives, according to Fox. “It’s good to get involved early with their care and make sure they’re plugged into the right providers,” he said. “It can be very fulfilling to watch these kids progress through school and graduate. It’s exciting to be part of their team.”
Learn more:
Cerebral Palsy Research Network
Cerebral Palsy Foundation



