3D printing process makes neurosurgical procedure more “real” for patient’s parents
Treating craniosynostosis is fairly routine for pediatric neurosurgeons. What made Paislee Schendel’s case unique for Carolina Sandoval, MD, was her collaboration with U of M radiologists David Nascene, MD, and Yu-Hui Huang, MD.
When Paislee was born, her parents, Chrissy and Austin, were concerned about her head shape. “The doctors told us that her head would likely round out, but it never did,” said Chrissy. “We went to a specialist at the end of January [2022] who confirmed that she had craniosynostosis. At that point, we were referred to Dr. Sandoval.”

Sandoval (pictured here), who practices at the Masonic Children’s Hospital in Minneapolis, met with Paislee’s family to go over her imaging and discuss surgical options. “She gave us the choice of having an earlier stage procedure using a minimally invasive approach or we could wait until Paislee was older and have the full surgery,” said Chrissy. “We chose the latter option.”
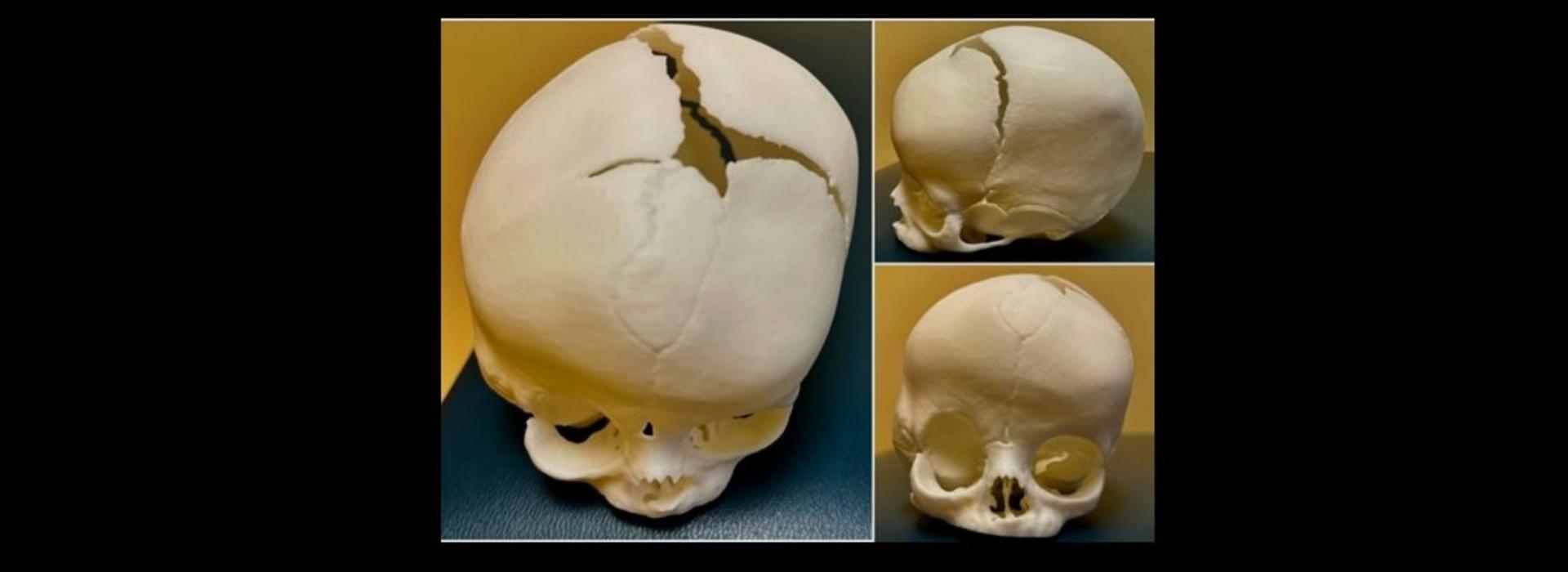
During the discussion about treatment approaches, Sandoval used a 3D model of Paislee’s skull to show Chrissy and Austin exactly what was wrong, and how it could be corrected. The model (pictured above) was printed by Drs. Nascene (pediatric neuroradiology) and Huang (radiology resident). It is based on Paislee’s CT scan, showing right-sided coronal craniosynostosis and demonstrating the extent of resulting orbital and cranial asymmetry, according to Sandoval.

“In 2017 I bought a 3D printer to tinker around with and had fun modeling and printing fixes to broken plastic bits around the house,” said Nascene (pictured here). “As a radiologist, it wasn't too long before I started converting data from imaging studies into 3D printable files. I wanted to create models of complex anatomical parts for trainees and patients that might be better understood by being held in their hands rather than read about in a book or online.”
Trainees in radiology have a tremendous amount of learning to do and Nascene is interested in making that learning a bit easier. “Sometimes a 3D-printed model can really help with tricky concepts,” he said.
Sandoval enthusiastically embraces Nascene’s skill with this technology. “The 3D models can help us preplan our surgical approach,” she said. “In Paislee’s case, however, the way the skull was to be reconstructed in the operating room was well established, so using the model wasn’t key for the surgical team. It did help with the parents because it enabled me to show them where the abnormalities were and how the plastic surgeon would cut the bones and remodel the cranial vault.”
Nascene has taken a special interest in craniosynostosis and the craniofacial population because reconstructing the abnormal skull creates a visually striking 3D construction, according to Sandoval. “He started a library of all the models of the different skull abnormalities that we see in our clinic,” she noted. “We use them for resident and student teaching.”
When using them for patient care, a surgeon could grab a marker and draw the operative plan right on the model and bring it into the OR to show the entire surgical team, according to Nascene. “My hope is that after planning with a model, the team will be better informed and the surgery will go smoother, saving OR time and reducing complications,” he added.
On April 25, 2022, Paislee had her reconstructive surgery, with Sandoval performing the neurosurgical portion of the procedure. “She did well during the surgery and had no complications postoperatively,” said Sandoval.
Chrissy and Austin agree. “It was scary, but it went really smoothly,” said Chrissy. “She recovered well – there were no bumps in the road.”
Paislee’s parents asked if they could keep a small version of her model. “It showed us what her skull wasn’t supposed to look like – it showed us what was wrong,” said Chrissy. “We saw it on paper, but the model made it real.”
Nascene and Huang want to use the 3D printing process to improve the delivery of healthcare and potentially get funding for it to be done for more patients, according to Sandoval. “For other physicians, particularly surgeons, I hope that the models we make will help them perform safer, quicker surgeries,” said Nascene. “Or perhaps even successfully plan a surgery they felt wasn't possible without the benefit of a model.”



