
U Study Focuses on Improving First-Line Treatment for Tourette Syndrome
Tourette Syndrome (TS) is a neurodevelopmental disorder, which is part of the spectrum of tic disorders and is characterized by motor and vocal tics. It is a relatively rare disorder that impacts around one percent of people and has varying degrees of impact on the quality of life of those affected. It often comes along with co-occurring emotional, behavioral and psychological difficulties that can add additional challenges to wellbeing and functioning. Unfortunately, right now there is no cure for TS, and the best treatments that exist only help around 50% of patients.
Christine Conelea, PhD, LP, an assistant professor in the Department of Psychiatry and Behavioral Sciences at the University of Minnesota Medical School, hopes to change that by finding new ways to improve those treatments so that more people benefit. She explains her research can be split into two buckets, saying, “One is trying to understand more about what factors cause or worsen symptoms, and the other is to improve the current treatments that we have.”
Testing Brain Function
To understand what factors cause or worsen symptoms in patients with TS, Dr. Conelea is testing brain function in different ways, especially among people who have TS and other common co-occurring disorders like ADHD and OCD. She says past research has tried studying people who only had TS, but because the syndrome is so rare, results have not been very informative.
Her lab does neuroimaging and computerized brain tests to try to figure out if there are better ways to identify how the brain is functioning in each individual patient. The hope is that they can use better neuroscience-based tools to measure a patient's brain function, and based on their profiles, make decisions about which treatment they should receive.
“With this information, we can develop treatments that more specifically target individual strengths and weaknesses. We are trying to figure out if there are better ways to match people to the treatment that is right for them,” Dr. Conelea said.
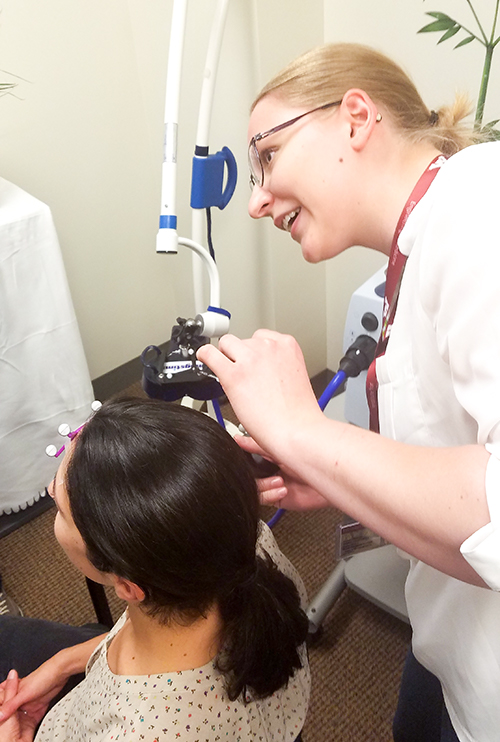
TMS and CBIT
Comprehensive Behavioral Intervention for Tics (CBIT) is a behavioral therapy that is currently the first-line treatment for patients that have tics. It involves teaching people to manage situations that make tics worse and develop specific skills for how to better control their tics. However, this type of treatment works well for only about half of the patients who receive it, so there is a need to improve how well CBIT works.
In the fall, Dr. Conelea’s lab will start a new study that will combine CBIT with transcranial magnetic stimulation (TMS). TMS works by holding a magnet over someone’s head and having electricity pulse through it that changes the activity in certain parts of the brain. TMS will be used in this study to change activity in a part of the brain that is involved in tics and overactive in people who have them.
“We will explore whether or not turning down activity in this area right before people practice the CBIT skills makes CBIT work better and faster for more people,” she said.
The TMS effects can last around half an hour after treatment, but participants in the study will get it every day for a couple of weeks to increase the after effect, which researchers predict will cause lasting brain change.
“By pairing TMS with therapy, we’re hoping to boost the brain’s ability to learn and retain therapy skills,” Dr. Conelea said.
Another challenge is that CBIT is not widely available. One thing Dr. Conelea is doing in collaboration with other TS researchers around the county is trying to do work on ways to improve CBIT and its access. They recently convened at the “Treating Tourette Together” summit at the University of Minnesota to learn how children and adults with TS, parents and healthcare providers would like researchers to improve CBIT. One idea they hope to pursue is increasing access to CBIT using telehealth.
Dr. Conelea hopes that between this outreach and her research efforts, soon patients will have new ways to treat their TS symptoms.
“Larger studies will be needed, but our hope that this work will lead to a new way of delivering CBIT in clinical care and a new non-invasive treatment option,” she said.



