Novel late-stage colorectal cancer treatment proves effective in preclinical models
University of Minnesota Medical School researchers say “tumor-secreted exosomes” help some cancer cells to evade immune response of current FDA-approved treatment options
MINNEAPOLIS/ST.PAUL (04/28/2021) — In a recent discovery by University of Minnesota Medical School, researchers uncovered a new way to potentially target and treat late-stage colorectal cancer – a disease that kills more than 50,000 people each year in the United States. The team identified a novel mechanism by which colorectal cancer cells evade an anti-tumor immune response, which helped them develop an exosome-based therapeutic strategy to potentially treat the disease.
“Late-stage colorectal cancer patients face enormous challenges with current treatment options. Most of the time, the patient’s immune system cannot efficiently fight against tumors, even with the help of the FDA-approved cancer immunotherapies,” said Subree Subramanian, PhD, an associate professor in the U of M Medical School’s Department of Surgery and a senior author of the study.
In partnership with Xianda Zhao, MD, PhD, a postdoctoral fellow in Subramanian’s laboratory, the duo set out to investigate how colorectal cancer becomes resistant to available immunotherapies. What they found was recently published in Gastroenterology, including:
-
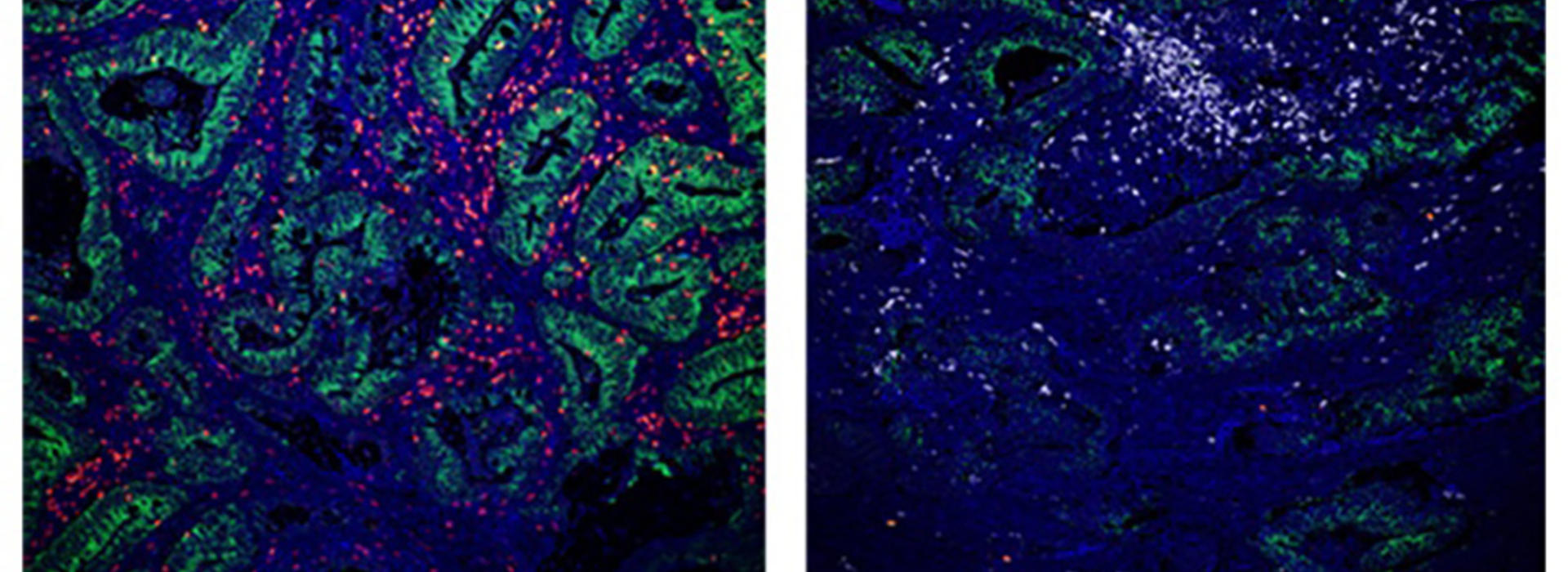
Colorectal cancer cells secrete exosomes that carry immunosuppressive microRNAs (miR-424) that actually prevent T cell and dendritic cell function because they block key proteins (CD28 and CD80) on these immune cell types, respectively. In the absence of these proteins, the T cells, which would normally kill the cancer cells, become ineffective and are eliminated from tumors, allowing tumors to grow.
-
By blocking these immunosuppressive microRNAs in cancer cells, the team observed an enhanced anti-tumor immune response and discovered that cancer cell-secreted exosomes also contain tumor-specific antigens that can stimulate the tumor-specific T cell response.
-
The researchers tested tumor-secreted exosomes without immunosuppressive microRNAs, in combination with immune checkpoint inhibitors, as a novel combination therapy in preclinical models with advanced-stage colorectal cancer, which proved effective.
“Our studies indicate that disrupting specific immunosuppressive factors in tumor cells helps unleash the immune system to effectively control tumor growth and metastasis in preclinical models with late-stage colorectal cancer,“ said Subramanian, who is also a member of the Masonic Cancer Center. “Eliminating the immune suppressive effects of those exosomes is now the focus of a new treatment option for patients with this deadly disease.”
The intellectual property behind the modified exosome technology has been protected with assistance from the U of M Technology Commercialization. The team is currently developing clinical-grade exosomes that can be tested in clinical trials for patients with colorectal cancer.
This work was supported by seed funding from Minnesota Colorectal Cancer Research Foundation, Mezin-Koats Colon Cancer Research funds and the University of Minnesota Medical School’s Department of Surgery.
###
About the University of Minnesota Medical School
The University of Minnesota Medical School is at the forefront of learning and discovery, transforming medical care and educating the next generation of physicians. Our graduates and faculty produce high-impact biomedical research and advance the practice of medicine. Visit med.umn.edu to learn how the University of Minnesota is innovating all aspects of medicine.
For media requests, please contact:
Angel Mendez
Media Relations Manager
mende434@umn.edu