A Team of U of M Faculty Designing Face Masks that Filter
About two weeks ago, Rumi Faizer, MD, dialed in to a call. An associate professor in the University of Minnesota Medical School’s Department of Surgery, he joined the line with dozens of other experts, including representatives from medical device companies, state leaders, physicians, design and engineering professors and more—all focused on solving a problem.
“Our healthcare personnel are terrified of seeing that point in the curve of COVID-19 where we don’t have enough PPE (personal protective equipment),” Dr. Faizer said.
One part of the PPE includes an N95 mask. It’s the best mask to protect healthcare professionals because of two reasons—its ability to filter out 95% of particles from the air (even as small as viruses) and its snug fit that encloses the breathing passageways and prevents particles from going in and out of gaps in the masks.
Because of various circumstances, the supply chain worldwide for these N95 masks is drying up, and the Department of Health and Human Services estimates that the U.S. will need 3.5 billion masks throughout the COVID-19 pandemic. That’s when leaders at the U initiated the call to action.
“In an ideal world, people would get an N95 and change it between every single patient,” Dr. Faizer said. “But in the real world, providers may get one N95 mask to use all day long as we ration PPE. Our designs are trying to bridge that gap, and we know the deadline is fast approaching.”
After seeing a video from the Boston Children’s Hospital while rounding, Dr. Faizer pulled a medical fellow aside to build and test the first prototype for an anesthesia mask.
“Within an hour of watching the video, we had validated that this stuff works,” he said. “That’s how this version of the technology that we’re working on today came to be, but we’ve made some upgrades to the design.”
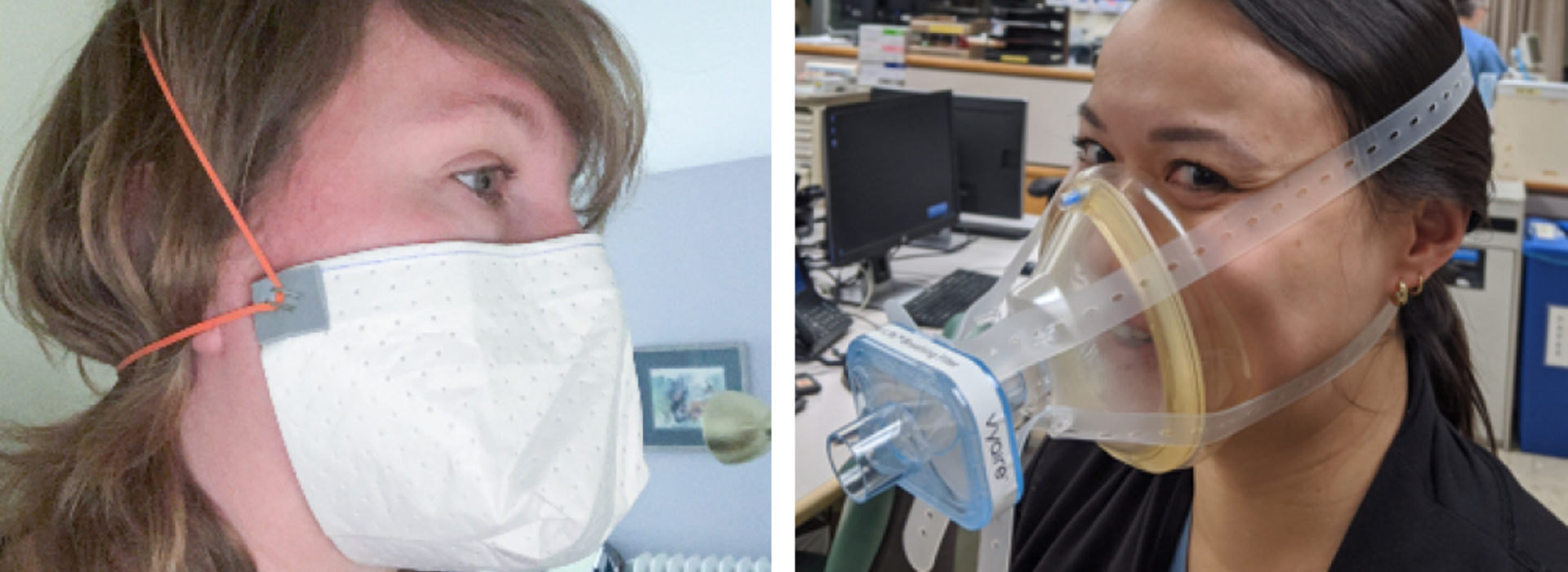
This design is one of two masks—one anesthesia mask and one single-use, disposable mask, called the Origami mask—both using special filtration material that Dr. Faizer and partnering U of M faculty say may be able to support local PPE demands.
Forming Critical Partnerships
On that pivotal, late March phone call, which was initiated by the U of M Institute for Engineering in Medicine’s (IEM) David Odde, PhD, Dr. Faizer connected with Linsey Griffin, PhD, an assistant professor in the College of Design, Will Durfee, PhD, professor in the College of Science and Engineering, along with a handful of other collaborators, who, together, have steered their two mask designs closer and closer to perfection using expertise from their respective fields.
“This couldn’t happen in one lab. This couldn’t happen in one department. This is an amazing effort across the Medical School, College of Science and Engineering, College of Design and beyond within the University,” said John Bischof, PhD, IEM director.
The partnership started with gaining an understanding of the key components of an N95 mask. David Pui, PhD, a Regents professor in the College of Science and Engineering and the director of the Center for Filtration Research (CFR), explained the need for these masks to contain a special type of filter with the capability to prevent a virus from seeping in or out of the mask.
“Nationally, there are shortages of those commercially available filters, and already for both masks, we’ve ordered what we could in terms of materials,” Dr. Faizer said.
Thankfully, connections between CFR faculty and corporate partner, Cummins, earned a critical donation from the global power leader—rolls of filtration material.
“Cummins was absolutely critical. Without that filter material, we would not have these masks. We would still be where we were two weeks ago,” Dr. Griffin said.
Establishing Fit and Filtration
Within 12 hours after receiving the Cummins filtration material, the team had early results on both mask prototypes. Dr. Pui’s lab ran tests on the material and found that it had potential for making face masks with the ability to filter out small particles.
“Then, the next part is determining if stuff can slip by through gaps in the mask,” Dr. Faizer added. “The way that’s done is through fit testing. You put this big hood on and they spray an aerosolized substance with a bad taste in it, which is made up of very small particles. If you have the mask on and you can taste it while moving and doing various maneuvers, then you know stuff is slipping through your mask. We’ve been doing that exact test to validate these masks.”
Fit is Dr. Griffin’s area of expertise. She leads the Human Dimensioning Lab, which focuses on understanding how to improve body-product relationships, specifically in wearable medical products, like personal protective equipment.
“That’s where my specialty lies,” Dr. Griffin said. “The measurements of our body are unique to us as individuals, so anytime you’re trying to create a product to fit a wide variety of faces, you have to really be cognizant of integrating a lot of adjustability features.”
Passing the Tests

The anesthesia mask has performed well on filtration and fit tests. Dr. Faizer says it can be kept clean and reused, but it still has its challenges.
“I’m sure I’ve scared a few people walking down the hallways with some of these anesthesia masks,” Dr. Faizer joked. “It does have limitations in terms of how comfortable it is to wear long-term and not being able to speak loudly through it, so we’d like for Linsey’s design to be the first line out there.”
That design, coined the origami mask, remains in the fit testing stage. Led by Dr. Griffin, the mask resembles closer to the traditional, single-use N95 masks. Since receiving the Cummins’ filtration material, she’s designed more than 80 masks, each time inching closer to the perfect fit.
“One of the challenges with these masks is that it can’t be sewn. Anytime you sew into the material, it’s puncturing a hole, which allows all of the particles that you’re trying to eliminate to come through,” she said. “We’re trying to figure out how we can use supplies that are on-hand to make this product and make this product fast.”
Dr. Griffin has kept the origami mask pattern simple, using only a handful of materials to create shape and comfort. Another donation from Bedford Industries provided bendable, wire-based material that serves as support for the nose.
“Right now, we’re really focused on how we can make this product even more adjustable to fit those faces that we’re currently not fitting. We’ve done three fit tests on this latest prototype, and we’re close.”
Preparing for Mass Production
While some built the masks, others took the lead in conceptualizing the next steps—production, sterilization and delivery. Dr. Griffin says the production site will operate within a large studio space inside McNeal Hall.
“Right now, we’re trying to build out the workflow of what production will look like with social distancing, so how many people can we have in a space, how do we manage the flow of people, the flow of product from workstation to workstation, all while making sure that we’re maintaining quality throughout the process,” she said.
The team plans to start production with a small group of people to streamline the process. As production becomes more seamless, they expect to train and add in more people until they are operating at their maximum level of production.
“Normally, no one would accept what we’re doing,” Dr. Faizer said. “You’d say, ‘Everything has to go up through multiple rounds of testing on a federal level before I’m putting anything on my face.’ The reality is we can’t afford that time, but the idea of a community of people putting together a bunch of masks and giving them out is incredibly nerve-wracking if you’re the nurse or the physician. We’re trying to take that fear out of the equation.”
“And, that’s why we are focused on protection,” Dr. Griffin added. “We want physicians, nurses and any healthcare workers to have the confidence that what they’re wearing is going to protect them. Because of that, we are being very rigorous with our testing and designs, but once we do nail down this single-use design, we’ve designed it for the purpose of mass producing it.”
To read more about the donation from Cummins, visit this webpage.