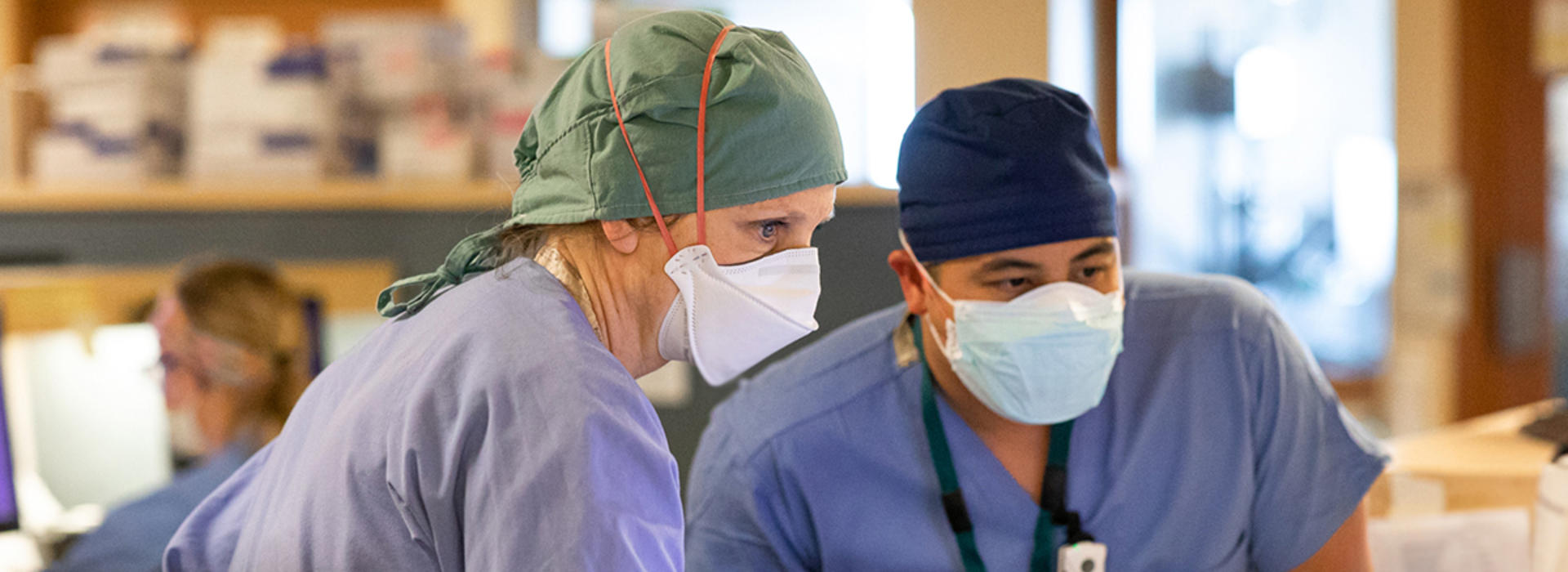
At the Speed of ‘Pandemic’
At the Speed of ‘Pandemic’
Which Emerging, Expeditious Processes for Clinical Trials the U of M Medical School will Keep and Grow
Read time: 5 minutes
After hearing about the first U.S.-based COVID-19 case, for some, it probably felt like mere hours later that hospitals struggled to find beds, positive cases quickly spiked and everyone sheltered at home indefinitely. The panic of a pandemic settled in faster than comprehension.
But, physicians and scientists around the world likely battled daily against their innate desires to fear and worry to, instead, focus on solutions that would save the lives of their patients. How, though, could medicine and science even begin to match the speed of the pandemic? The process of taking clinical findings from the research bench to the bedside is not known for its haste. In fact, research shows that, on average, it takes 17 years for research to reach clinical practice.

“It’s a problem, and we have had to think creatively this last year about how to overcome this to provide real-time care for our patients,” said Brad Benson, MD, professor in the Departments of Medicine and Pediatrics at the University of Minnesota Medical School and chief academic officer for M Health Fairview. “Our state’s first and only cohorted COVID-19 hospital was the result of that creative thinking and soon became a place where bedside care teams and principle investigators directly collaborated to discover better ways to treat this disease. This process has proven that we can efficiently conduct clinical trials, from approval to completed accrual, in much shorter times than we’ve historically seen. The lessons learned should change the way we do things in the future.”
He shares three themes from the past year that have permanently shortened the time frame between making clinical findings and improving patient care between the U of M Medical School and within the M Health Fairview system:
Develop a shared purpose
Communicate systematically
Leverage big data and technology
Develop a shared purpose
Before COVID-19, M Health Fairview embraced adding “new research participant accruals” as a sixth key performance indicator by which leadership would be judged. The team set it 10% higher than 2019 totals. Then, the pandemic began. By the end of 2020, 26 COVID-19 clinical trials alone had shattered the year’s expectations, and coupled with nearly 1,000 other clinical trials already in progress within the health system, totals for 2020 had reached a record-breaking 41% growth over 2019.
“We have such a strong shared purpose within the partnership for research that we became a health system committed to having research metrics as one of our key performance indicators,” Dr. Benson says. “We had a deep pool of scientists who were ready and able to pivot quickly, and we had leaders that supported this in every way. So, when COVID-19 hit, we were all already focused – from the bedside providers to our research teams – so that all the traditional barriers to getting research done, melted away.”
Dr. Benson joined a few other leaders within the M Health Fairview system who became the first stop for all COVID-19 research proposals.
"Because we have the 40,000-foot view of what resources are available, and all of the different things that are going on in the organization, this team reviews all of the research before it begins,” Dr. Benson says. “We have a special category for COVID-19 research, given that it is so critical to providing insight and best care for our patients, and it is fast-tracked. This has removed any barriers and immediately brings resources to bear."
Communicate systematically
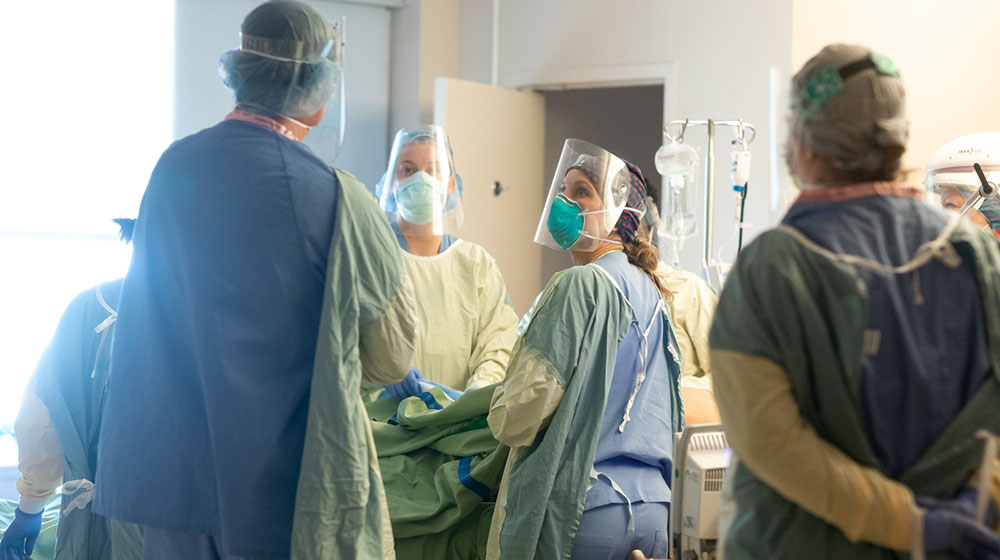
With no known therapy or cure in sight, providers around the world struggled, at first, to understand the best course of care for their patients with COVID-19. Dr. Benson recalls his team “being bombarded” by potential treatments, causing added stress and confusion in an already burdened clinical environment. So, his team developed a few methods to communicate about research systematically.
“To help them, we leveraged a team who put together evidence-based reviews of what works, what doesn't work and what we, as a system, would support in terms of treatment,” he says. “And, the research we do approve, we make sure is additive – not intrusive – to the bedside team’s care.”
To do that, Dr. Benson says the bedside teams meet directly with the principal investigators of any COVID-19 study in an effort to problem-solve and collaborate weekly. And, daily, the M Health Fairview leadership team addresses any research issue by 10 a.m.
"Our health system has initiated daily huddles that begin at 7 a.m. every day. And, if a problem arises in that huddle that can’t be solved, it escalates to the next huddle,” Dr. Benson says. “If there's a problem that has percolated up in each of the five layers of huddles that hasn't been solved yet, then there's a plan for it by 10 a.m., which is discussed in the senior executive huddle. For anything that might impact care, research or education, that communication is absolutely critical and something we will continue to use post-pandemic."
Leveraging big data and technology
M Health Fairview led the way in COVID-19 patient care by setting up one of the nation’s first – and Minnesota’s only – cohorted COVID-19 hospital.
“Because of this, we are able to offer new, potential therapies and care to folks in a rapid way, but it also helped us develop our own in-house database critical to our research,” Dr. Benson says. “We have leveraged some of the University of Minnesota’s world-class data scientists who made it possible for us to ask and answer questions early on that fueled our research.”
Researchers within the M Health Fairview system also worked with UnitedHealth Group out of Minnetonka, Minn., who had the world’s largest COVID-19 patient database. This partnership led to several critical insights into potential COVID-19 treatments, helping launch a multi-site trial – led by the U of M Medical School – that’s currently investigating the use of metformin as an outpatient treatment to prevent hospitalization of patients recently infected with SARS-CoV-2.
"We have used advanced data science techniques to identify the people who were on certain medications, found that maybe a good chunk of them ended up not being hospitalized and then studied that medication,” Dr. Benson says. “And, some of our clinical trials are even offered internationally thanks to remote-consenting with study participants, Zoom and access to electronic health records."
This data and other technology provided additional support in helping allocate scarce resources.
"Within our hospital, we developed a scoring system for who is at lowest and highest risk of serious disease from COVID-19, so that in the emergency room, it gives clinicians immediate decision support as soon as the patient’s positive test pops up,” he says. “This gives us a heads up on those who may look great at the time of diagnosis but have a high likelihood of getting really sick. We’ve been able to enroll them in a program that contacts them daily to ensure they are not progressing and get them in quickly if they do worsen. Our patients and families have appreciated that connection."
Dr. Benson emphasizes that institutions with the ability to adopt a “learning health system” approach – where scientists are built into the care delivery process – will thrive in a post-pandemic research world.
“We are only able to move as nimbly and quickly as we do because we are set up to either succeed or fail rapidly, and then learn from it,” he says. “It truly allows us to quickly make decisions, resolve any barriers to research and come together not just for the patient in front of us but also a world that is reeling from COVID-19. We’ve learned that what moves us, which is making the world a better place one patient, one learner, one discovery at a time, is best achieved when we do it together.”
University of Minnesota Medical School launches clinical trial studying metformin treatment for COVID-19
A new multi-site clinical trial led by the University of Minnesota Medical School is studying the effectiveness of metformin, a generic medication for type 2 diabetes, in the treatment of COVID-19. It will be the first randomized clinical trial for COVID-19 in the world to include pregnant women.
For Early Treatment of Mild COVID-19, University of Minnesota Trial Shows Hydroxychloroquine Has No Benefit Over Placebo
The trial results, published in the Annals of Internal Medicine, determined that hydroxychloroquine did not decrease the severity of COVID-19 symptoms over 14 days any better than a placebo.
University of Minnesota Medical School launches COVID-19 vaccine trial
The clinical trial, which closed in February 2021, is testing the safety and effectiveness of an investigational vaccine developed by U.S. biotechnology company Novavax, Inc., called NVX-CoV2373. Novavax is a late-stage biotechnology company developing next-generation vaccines for serious infectious diseases.
University of Minnesota expands clinical investigation of engineered iPSC-derived NK cells, opening U.S. clinical trial for the treatment of COVID-19
The first patient has received treatment in a new clinical trial that has opened at the University of Minnesota to test whether a novel cell therapy currently under clinical investigation as a treatment for acute myeloid leukemia (AML) and lymphoma can be effective as a treatment for COVID-19.